Diabetes Prenatal: Your Essential Guide to a Healthy Pregnancy
If you've recently been diagnosed with high blood sugar during pregnancy, or if you had diabetes before you became pregnant, you are likely feeling overwhelmed. You are not alone! Navigating pregnancy while managing a health condition like diabetes requires extra care, but it is entirely manageable with the right knowledge and support.
This guide is designed to break down everything you need to know about Diabetes Prenatal management in a way that is easy to understand. We will cover risks, management strategies, and what to expect during your prenatal journey, ensuring you feel empowered and prepared for the arrival of your little one.
Understanding What Diabetes Prenatal Truly Means
When we talk about Diabetes Prenatal, we are referring to any type of diabetes that affects a woman before or during pregnancy. This usually falls into two main categories: Pre-existing Diabetes (Type 1 or Type 2) and Gestational Diabetes (GDM), which develops specifically during pregnancy.
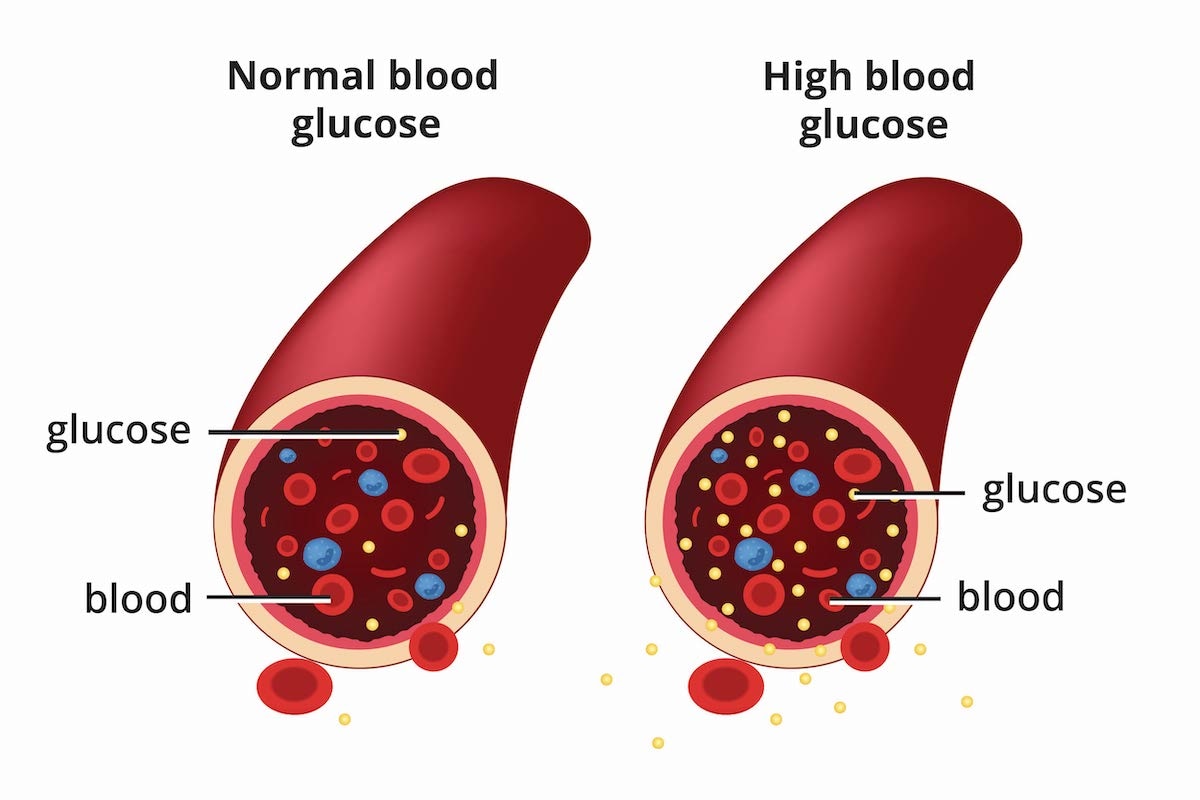
Regardless of the type, the core issue remains the same: high blood glucose levels. During pregnancy, maintaining tight control over your blood sugar is crucial because glucose freely crosses the placenta, directly affecting the baby's growth and development.
The good news is that medical advancements mean most women with prenatal diabetes can have healthy, full-term pregnancies. Success hinges on rigorous monitoring, consistent communication with your healthcare team, and making proactive lifestyle changes.
Who is at Risk for Diabetes Prenatal?
While Gestational Diabetes can affect anyone, certain factors increase your likelihood of developing it. If you have pre-existing Type 1 or Type 2 diabetes, your primary focus will be optimizing your current treatment plan to meet the demands of pregnancy. However, if you are being screened for GDM, your doctor will look closely at your medical history.
Common risk factors for developing GDM include:
- Being overweight or obese before pregnancy.
- Having a family history of Type 2 diabetes.
- Being diagnosed with GDM in a previous pregnancy.
- Being over the age of 25.
- Having Polycystic Ovary Syndrome (PCOS).
- Having previously delivered a baby weighing more than 9 pounds.
If any of these apply to you, your doctor may recommend earlier or more frequent screenings. Early detection is a powerful tool in managing Diabetes Prenatal successfully.
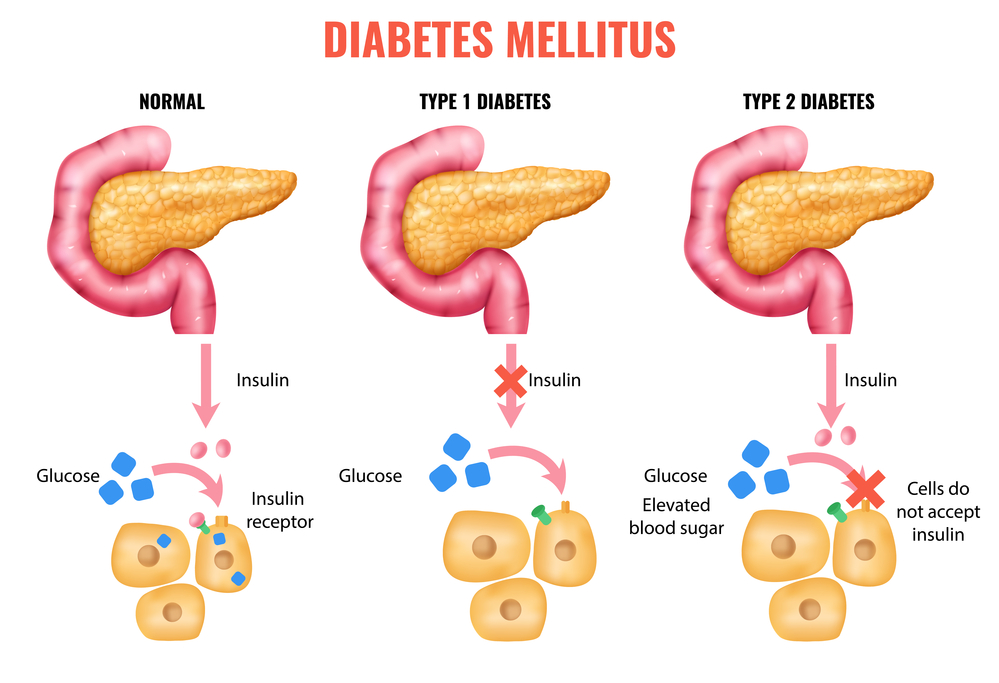
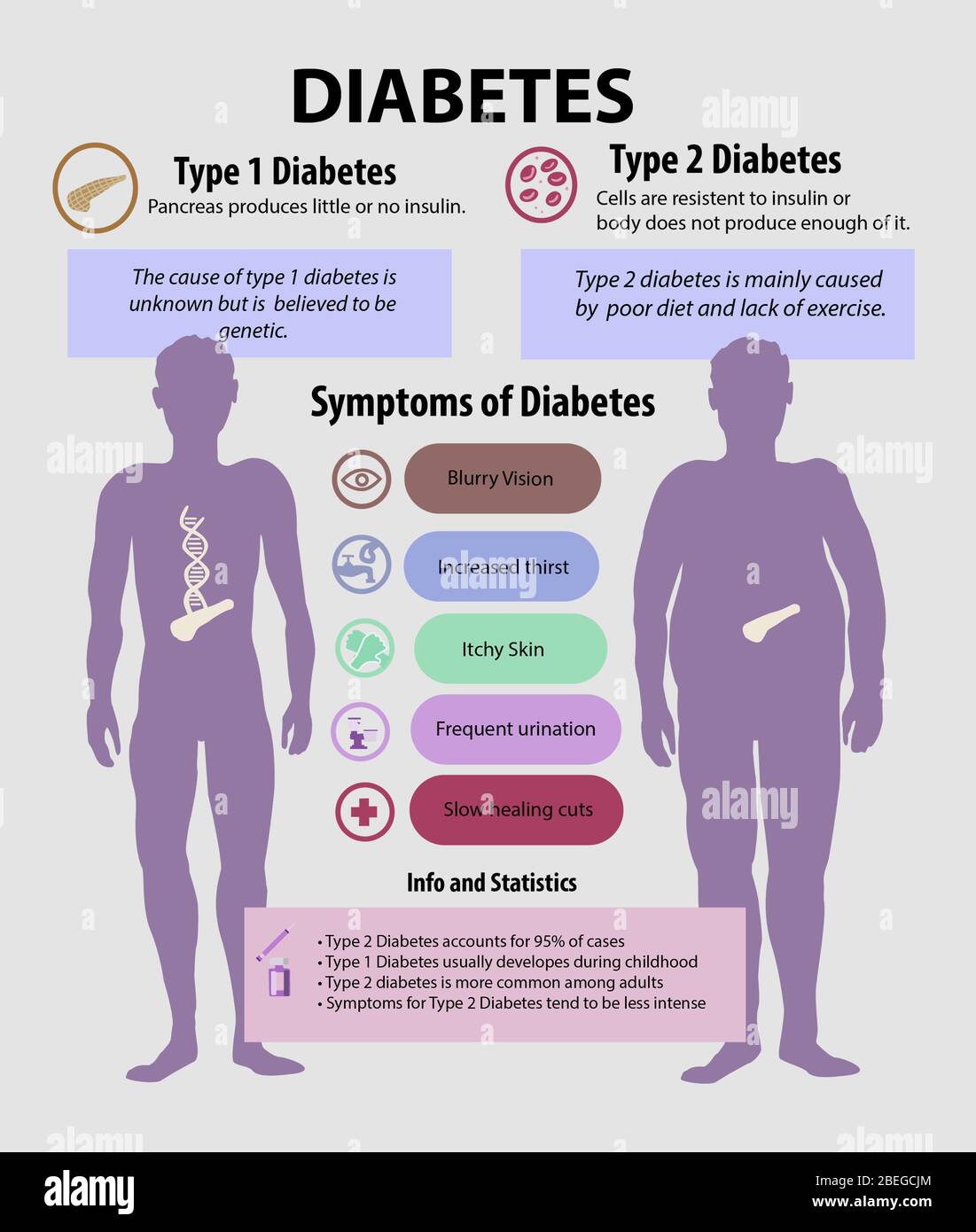
The Difference Between Type 1, Type 2, and Gestational Diabetes
It's important to clarify the definitions, as the long-term implications and immediate treatment plans vary depending on the type of diabetes you are dealing with during the prenatal period.
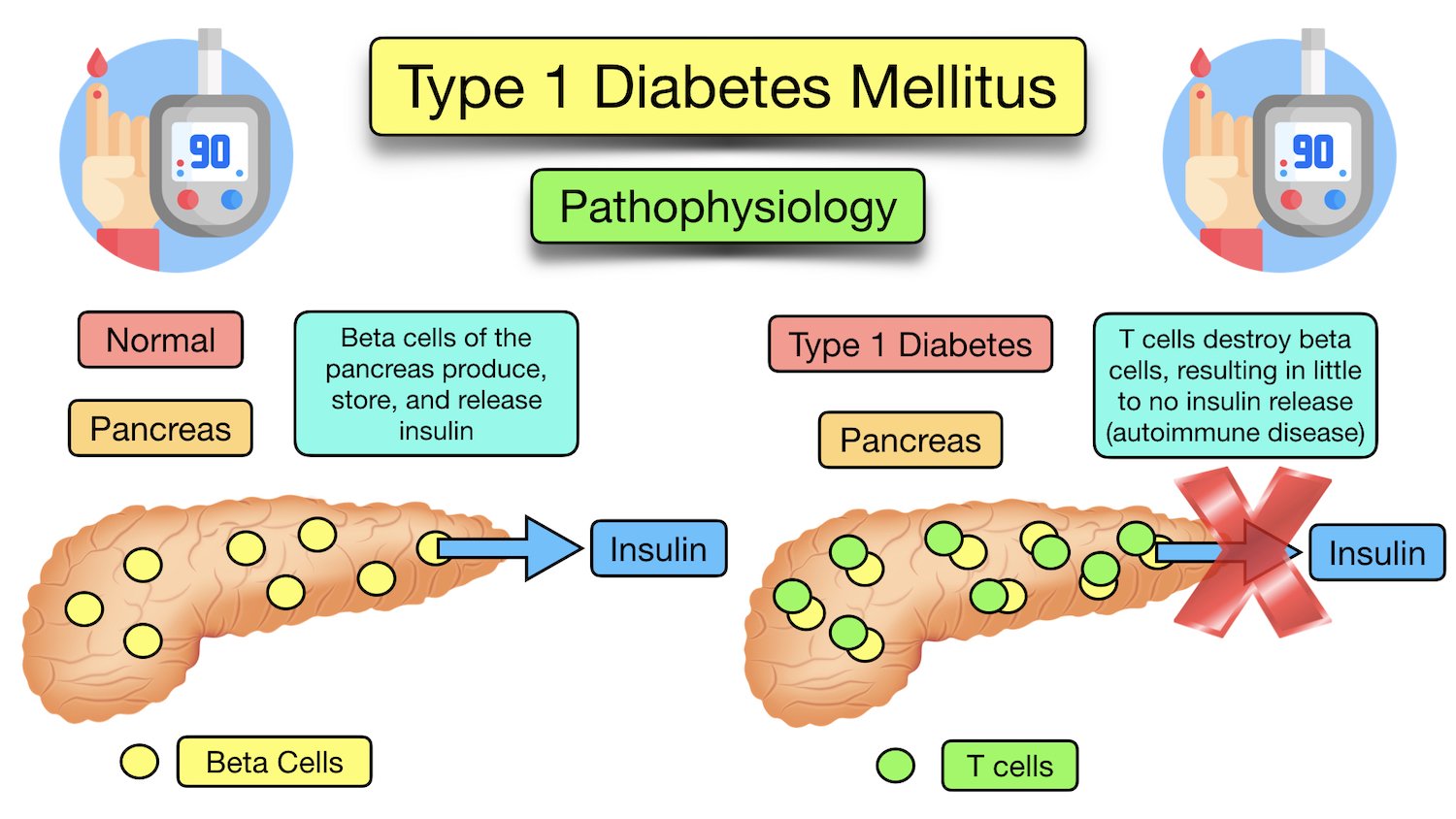
Type 1 Diabetes (T1D): This is an autoimmune condition where the body does not produce insulin. If you have T1D, managing pregnancy involves meticulous insulin dosing adjustments, as your insulin needs will drastically increase as the pregnancy progresses.
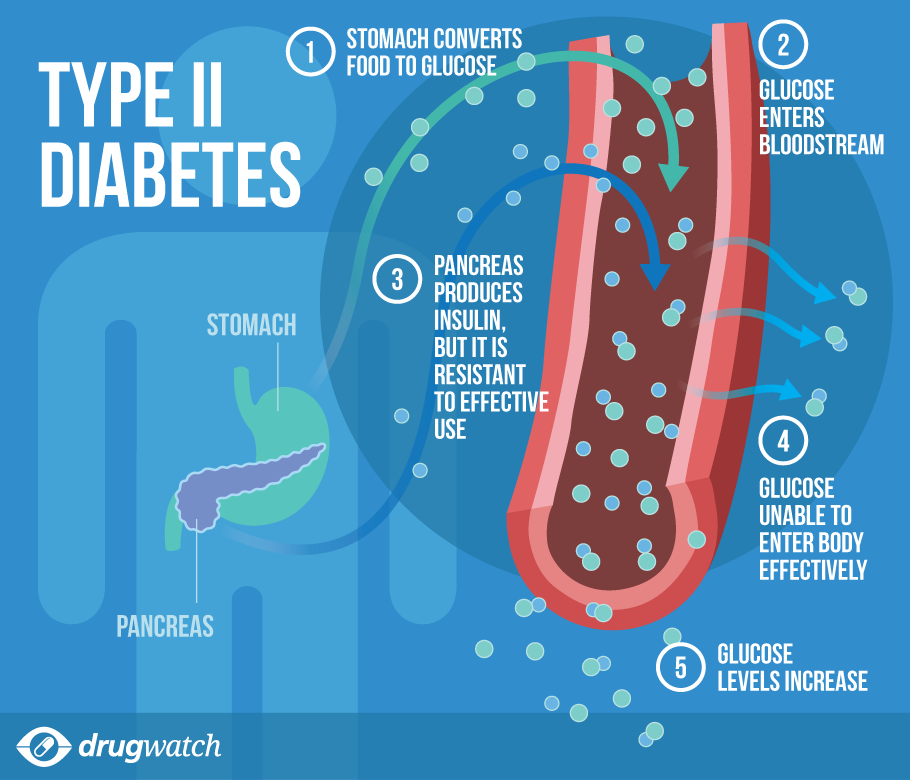
Type 2 Diabetes (T2D): This usually involves insulin resistance and sometimes insufficient insulin production. Management often requires transitioning off oral medications that are unsafe during pregnancy and relying more heavily on diet, exercise, and often, insulin injections.
Gestational Diabetes Mellitus (GDM): This occurs when pregnancy hormones interfere with the body's ability to use insulin effectively (insulin resistance). GDM usually resolves shortly after birth, though having GDM increases your risk for developing Type 2 diabetes later in life.
Managing Your Blood Sugar Levels: Lifestyle Adjustments
Whether you have pre-existing Diabetes Prenatal or GDM, the first line of defense is always lifestyle modification. Taking control of your diet and exercise routine can significantly impact your blood sugar stability and may reduce the need for medication.
Remember that managing your blood sugar is a team effort. You will likely be working closely with a dietitian (Registered Dietitian Nutritionist, RDN) and possibly a Certified Diabetes Care and Education Specialist (CDCES) to tailor a plan that works specifically for your pregnancy needs.
Dietary Changes: Eating for Two (Safely)
Dietary management is perhaps the most powerful tool in controlling blood glucose during pregnancy. The goal isn't to restrict calories, but rather to balance your nutrient intake and manage carbohydrate consumption effectively throughout the day.
Here are key strategies for managing your diet with Diabetes Prenatal:
- Consistent Carbohydrate Intake: Instead of eating a large amount of carbohydrates at once, distribute them evenly across three meals and two to three snacks daily. This prevents spikes and keeps energy levels steady.
- Focus on High Fiber: Choose complex carbohydrates like whole grains, legumes, fruits, and non-starchy vegetables. Fiber slows down glucose absorption, helping to stabilize blood sugar.
- Prioritize Protein and Healthy Fats: Always pair carbohydrates with a source of protein (like lean meat, eggs, or nuts) or healthy fat (like avocado or olive oil). This combination further minimizes post-meal blood sugar surges.
- Avoid Sugary Beverages: Eliminate sodas, juices, and sweetened teas. These deliver a quick, concentrated hit of sugar that is difficult to manage during pregnancy.
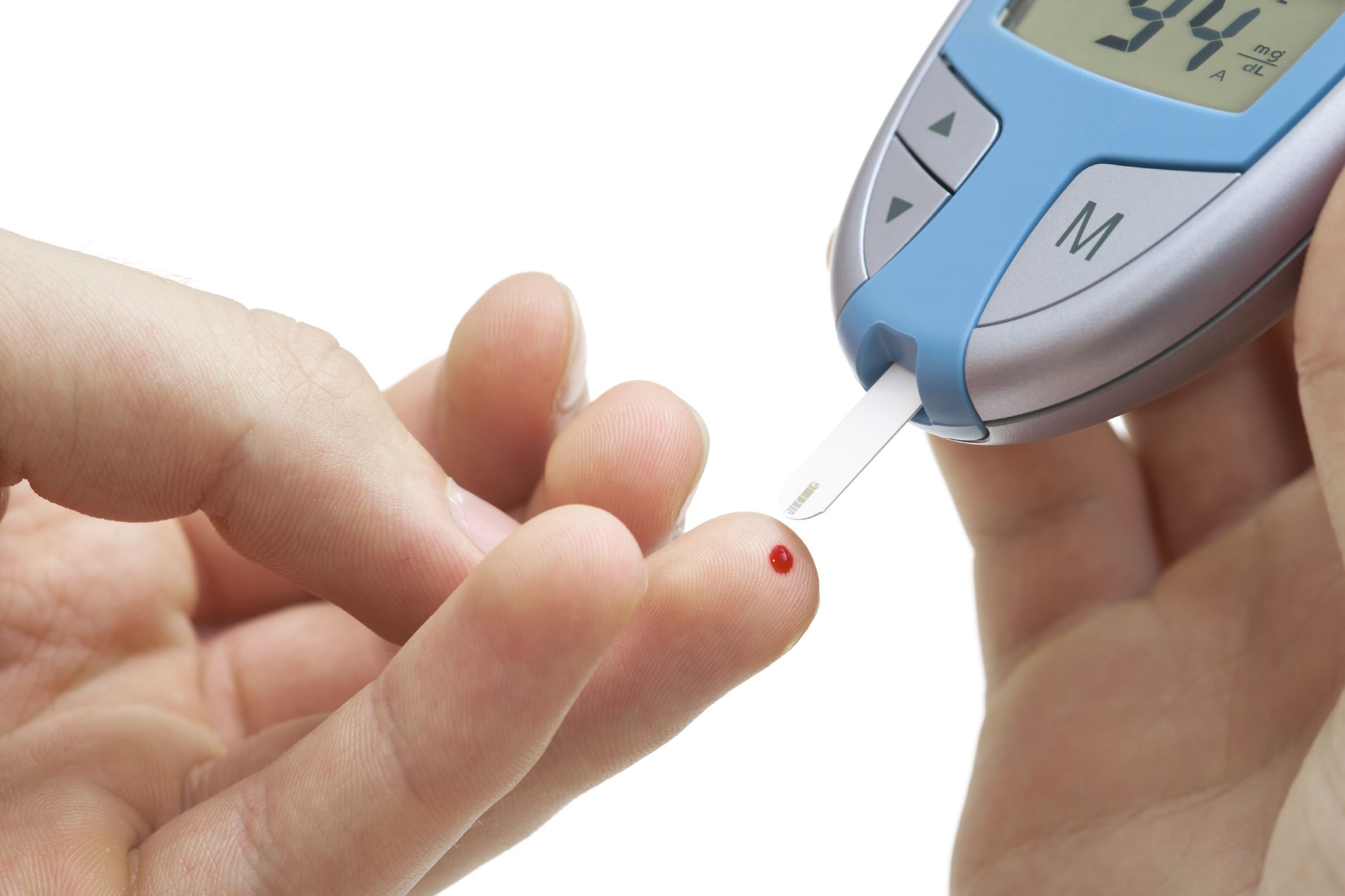
Remember to always monitor your blood sugar one or two hours after eating to see how specific foods affect you. Everyone is different, and tracking helps you identify your personal dietary triggers.
The Role of Exercise in Diabetes Prenatal Management
Physical activity is incredibly beneficial for pregnant women, especially those managing diabetes. Exercise increases your cells' sensitivity to insulin, meaning your body can use the available insulin more effectively to lower blood sugar.
Even moderate activity can make a huge difference. Aim for at least 30 minutes of moderate-intensity activity most days of the week. Post-meal walks are particularly effective because they help process the glucose from the food you just ate.
Safe prenatal exercise options include:
- Brisk walking or light jogging (if you were jogging prior to pregnancy).
- Swimming and water aerobics.
- Prenatal yoga or Pilates.
- Cycling on a stationary bike.
Before starting any new exercise routine, make sure you discuss it with your obstetrician. They can help ensure the activities are appropriate for your stage of pregnancy and overall health condition.
Potential Risks and Monitoring During Diabetes Prenatal
When blood glucose levels are consistently high, both the mother and baby face increased risks. For the baby, uncontrolled Diabetes Prenatal can lead to macrosomia (excessive birth weight), prematurity, respiratory issues, and hypoglycemia shortly after birth. For the mother, risks include preeclampsia and the potential need for a C-section.
However, this is why strict monitoring and management are essential! Your healthcare team will likely increase the frequency of your prenatal visits and may incorporate specialized monitoring techniques to ensure the baby is thriving.
Fetal Monitoring and What to Expect
Starting around the third trimester (often earlier for Type 1 and Type 2 diabetes), your doctor will implement additional tests to monitor the baby's well-being and assess placental function. These specialized tests provide reassurance and guide timing for delivery.
Key monitoring procedures include:
- Non-Stress Test (NST): This test measures the baby's heart rate in response to movement, checking for sufficient oxygen supply.
- Biophysical Profile (BPP): This combines an ultrasound with an NST. It assesses the baby's breathing, movement, muscle tone, and the amount of amniotic fluid.
- Detailed Ultrasounds: These are used frequently to monitor the baby's growth rate and size, specifically looking for signs of macrosomia.
These extra tests are simply precautions to ensure that your carefully managed blood sugar levels are translating into a healthy environment for your growing baby. Embrace them as opportunities to see your little one more often!
Navigating pregnancy with diabetes is certainly challenging, but it is a temporary season that yields the greatest reward. Stay committed to your monitoring plan, rely on your healthcare team, and be proud of the dedication you show every day to the health of your baby.
Conclusion
Managing Diabetes Prenatal, whether it's a pre-existing condition or Gestational Diabetes, demands vigilance but offers tremendous control over outcomes. By committing to a balanced diet, consistent physical activity, and meticulous blood glucose monitoring, you are taking the most crucial steps toward a healthy, successful pregnancy.
Do not hesitate to leverage the support systems available—your endocrinologist, dietitian, obstetrician, and family are all part of your team. Remember that every successful day of maintaining target glucose levels is a victory for both you and your baby. Stay positive, stay informed, and enjoy this incredible journey!
Frequently Asked Questions (FAQ) About Diabetes Prenatal
- What are the target blood sugar ranges during pregnancy?
- Targets can vary slightly depending on your specific situation, but generally, the American Diabetes Association recommends fasting glucose levels below 95 mg/dL, and one-hour post-meal levels below 140 mg/dL, or two-hour post-meal levels below 120 mg/dL.
- Will my baby automatically have diabetes if I have Diabetes Prenatal?
- No. Gestational Diabetes (GDM) usually does not cause the baby to have diabetes, though poor control of GDM can increase the baby's risk of developing metabolic issues later in life. If you have Type 1 or Type 2 diabetes, there is a very slight increase in genetic predisposition, but it is not automatic.
- Do I need to check my blood sugar more often than non-diabetic pregnant women?
- Yes. You will likely be asked to check your glucose levels four or more times daily: fasting, and then one or two hours after each meal. This frequent monitoring is essential for making timely adjustments to diet or medication.
- What happens if my Gestational Diabetes doesn't go away after delivery?
- For most women, GDM resolves immediately after the baby is born. If it persists (which is rare), you will be diagnosed with Type 2 diabetes and will need continuous management. It is crucial to get re-tested six to twelve weeks postpartum to confirm the GDM has disappeared.
- Can I take oral diabetes medication during pregnancy?
- Insulin is the preferred and safest treatment for Diabetes Prenatal that cannot be managed by diet and exercise alone. While some doctors may prescribe certain oral medications (like Metformin or Glyburide) under specific circumstances, insulin remains the gold standard because it does not cross the placenta.
Diabetes Prenatal
Diabetes Prenatal Wallpapers
Collection of diabetes prenatal wallpapers for your desktop and mobile devices.
Dynamic Diabetes Prenatal Capture Digital Art
This gorgeous diabetes prenatal photo offers a breathtaking view, making it a perfect choice for your next wallpaper.
Gorgeous Diabetes Prenatal Moment for Desktop
Find inspiration with this unique diabetes prenatal illustration, crafted to provide a fresh look for your background.
Serene Diabetes Prenatal Design Photography
Experience the crisp clarity of this stunning diabetes prenatal image, available in high resolution for all your screens.
Spectacular Diabetes Prenatal View for Your Screen
Find inspiration with this unique diabetes prenatal illustration, crafted to provide a fresh look for your background.

Vivid Diabetes Prenatal Scene Nature
Transform your screen with this vivid diabetes prenatal artwork, a true masterpiece of digital design.
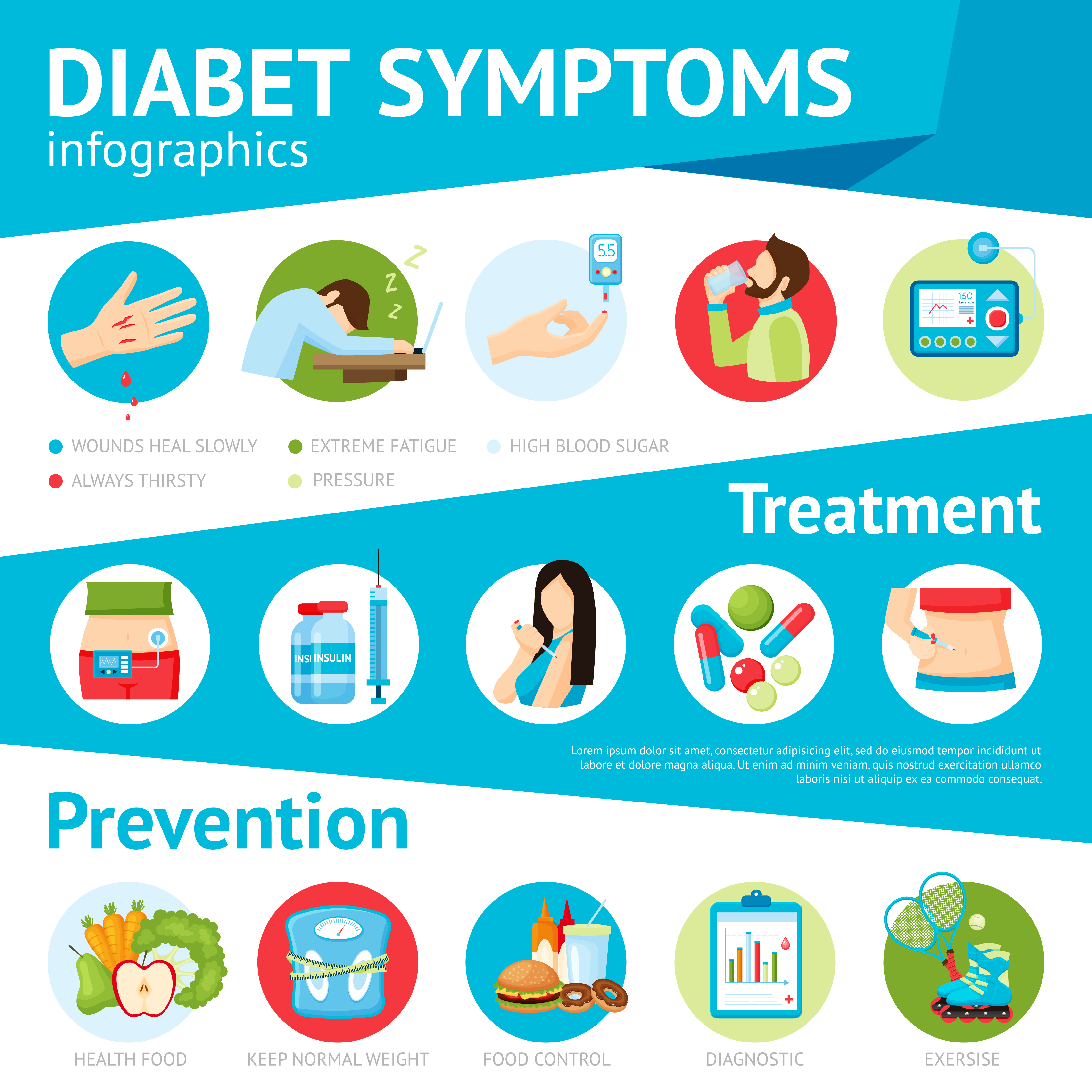
Dynamic Diabetes Prenatal Photo for Your Screen
This gorgeous diabetes prenatal photo offers a breathtaking view, making it a perfect choice for your next wallpaper.

Detailed Diabetes Prenatal Moment Art
Discover an amazing diabetes prenatal background image, ideal for personalizing your devices with vibrant colors and intricate designs.
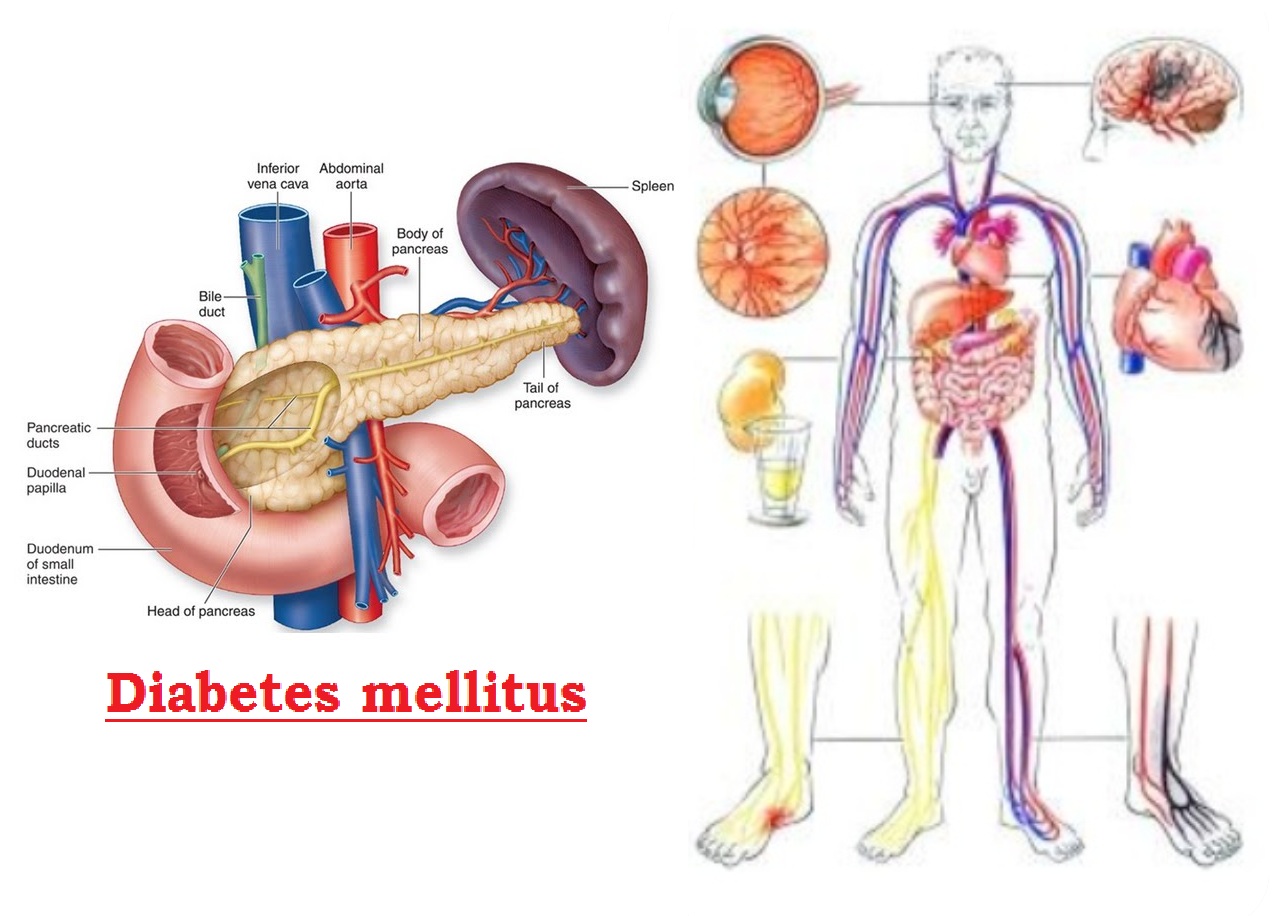
Breathtaking Diabetes Prenatal Artwork Photography
Experience the crisp clarity of this stunning diabetes prenatal image, available in high resolution for all your screens.
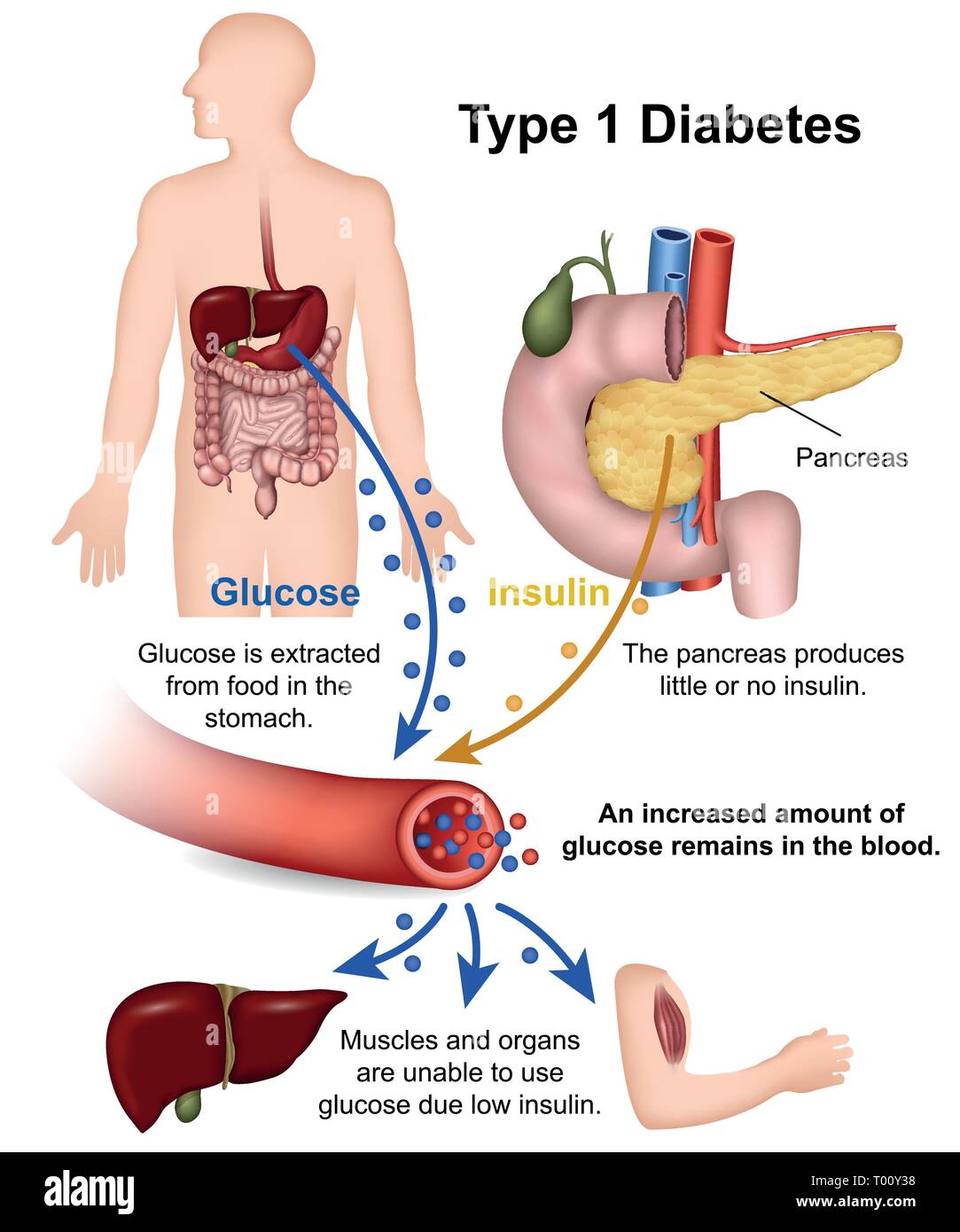
Gorgeous Diabetes Prenatal Picture in HD
Find inspiration with this unique diabetes prenatal illustration, crafted to provide a fresh look for your background.
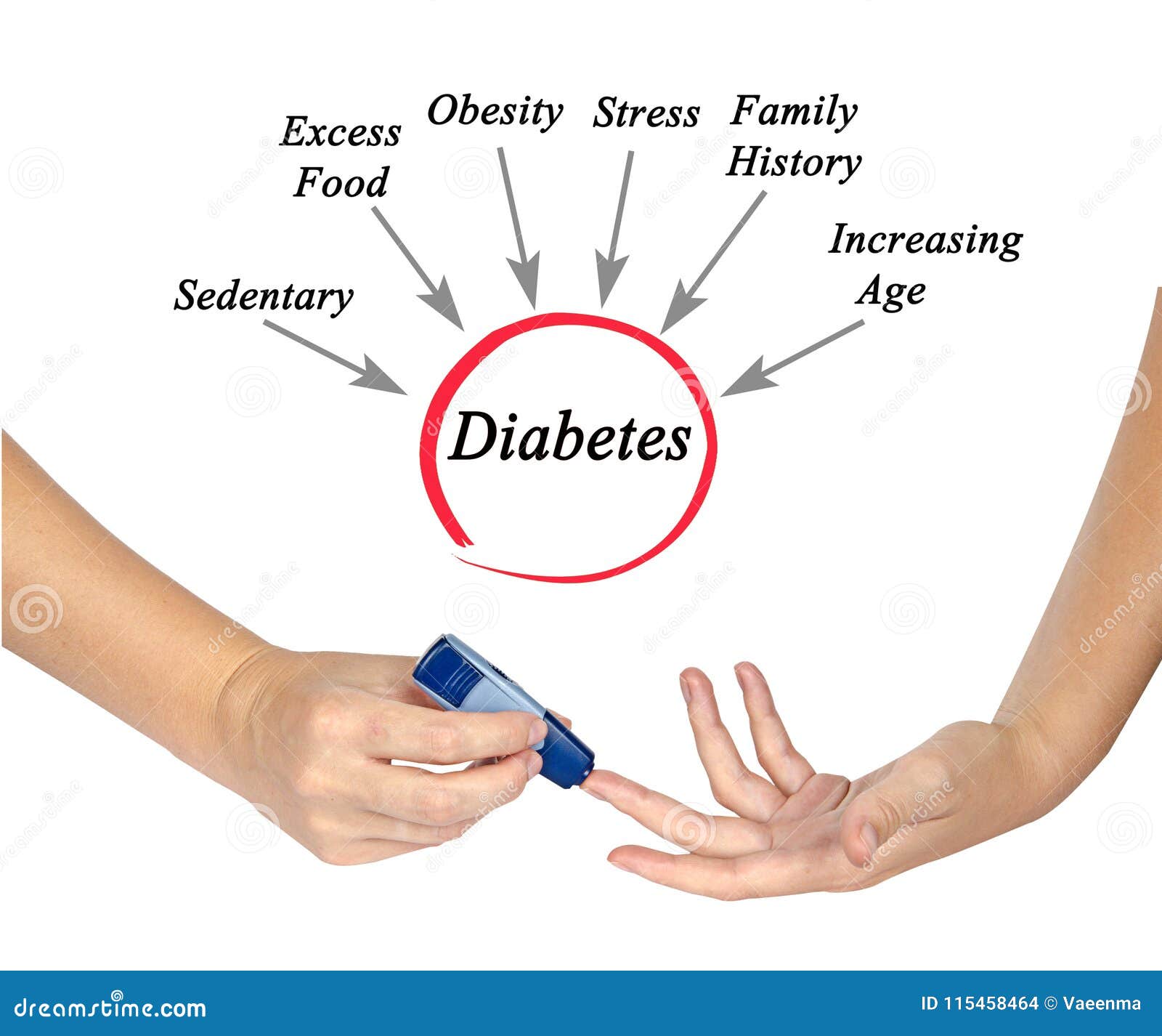
Serene Diabetes Prenatal Photo Collection
Explore this high-quality diabetes prenatal image, perfect for enhancing your desktop or mobile wallpaper.
/complicationsofdiabetes-GettyImages-1302948460-829d6ca13e4945eab127f8dd9d87b773.jpeg)
Beautiful Diabetes Prenatal View for Desktop
Transform your screen with this vivid diabetes prenatal artwork, a true masterpiece of digital design.
Lush Diabetes Prenatal Wallpaper for Your Screen
A captivating diabetes prenatal scene that brings tranquility and beauty to any device.
Beautiful Diabetes Prenatal Picture Art
Experience the crisp clarity of this stunning diabetes prenatal image, available in high resolution for all your screens.
Gorgeous Diabetes Prenatal Background Nature
Immerse yourself in the stunning details of this beautiful diabetes prenatal wallpaper, designed for a captivating visual experience.

Artistic Diabetes Prenatal View Collection
Immerse yourself in the stunning details of this beautiful diabetes prenatal wallpaper, designed for a captivating visual experience.

Exquisite Diabetes Prenatal Image Collection
This gorgeous diabetes prenatal photo offers a breathtaking view, making it a perfect choice for your next wallpaper.
Vivid Diabetes Prenatal Capture Illustration
Transform your screen with this vivid diabetes prenatal artwork, a true masterpiece of digital design.

Gorgeous Diabetes Prenatal Wallpaper in 4K
A captivating diabetes prenatal scene that brings tranquility and beauty to any device.
Vivid Diabetes Prenatal Design for Mobile
Experience the crisp clarity of this stunning diabetes prenatal image, available in high resolution for all your screens.

Gorgeous Diabetes Prenatal Abstract for Mobile
A captivating diabetes prenatal scene that brings tranquility and beauty to any device.
Download these diabetes prenatal wallpapers for free and use them on your desktop or mobile devices.