About Type 2 Diabetes: Your Essential Guide to Understanding and Managing It
If you're reading this, you might be feeling overwhelmed or maybe just curious about Type 2 Diabetes. Don't worry, you are absolutely not alone. Millions of people around the world live healthy, fulfilling lives while managing this condition. Our goal today is simple: to break down everything you need to know in a friendly, easy-to-digest way.
Think of this article as a supportive chat, covering what Type 2 Diabetes is, why it happens, and—most importantly—how you can take charge of your health. Understanding the basics is the first crucial step toward effective management and peace of mind. Let's dive right in and tackle this together!
What Exactly is Type 2 Diabetes?
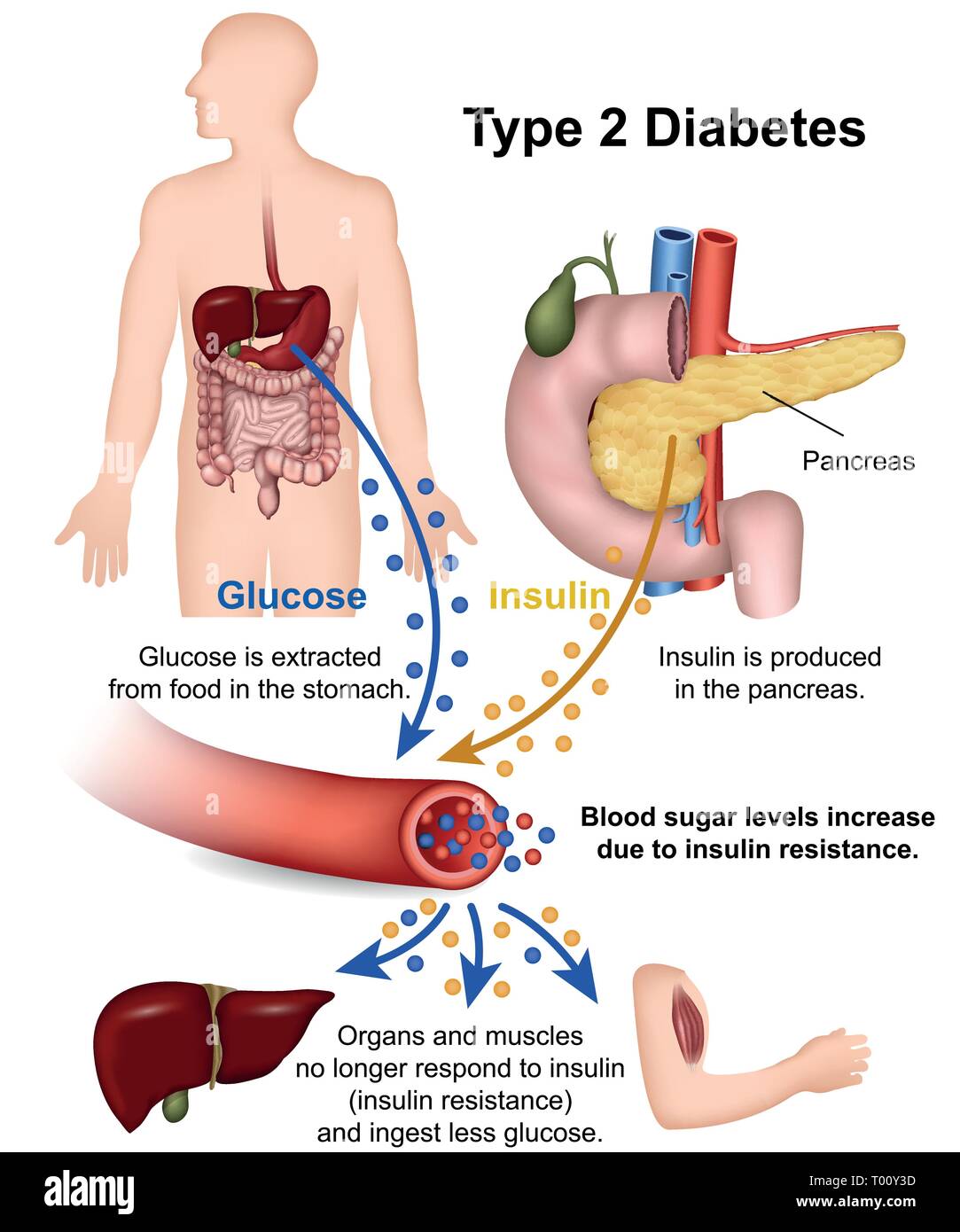
At its core, Type 2 Diabetes is a condition where your body doesn't handle sugar (glucose) properly. Glucose is your body's main source of energy, and it comes from the food you eat. To get that glucose into your cells, you need insulin—a hormone produced by your pancreas.
In people with Type 2 Diabetes, two main problems occur. Firstly, your cells become resistant to insulin. This means the insulin is there, but the cells aren't listening properly, a state known as insulin resistance. Secondly, over time, the pancreas can't produce enough insulin to overcome this resistance.
As a result of these issues, glucose builds up in your bloodstream instead of fueling your cells. This elevated level of blood sugar is what causes health problems over time. Therefore, managing Type 2 Diabetes essentially means keeping that blood sugar level within a healthy target range.
The Roots: Why Does Type 2 Diabetes Happen?
Type 2 Diabetes usually develops gradually, and it's often a combination of genetic predisposition and lifestyle factors. While genetics load the gun, lifestyle often pulls the trigger, making the body less efficient at using insulin.
Understanding the common risk factors can help you gauge your own vulnerability and motivate preventive action. Although having one risk factor doesn't guarantee the disease, multiple risk factors significantly increase the odds.
Here are the key factors contributing to the development of Type 2 Diabetes:
- Excess Weight or Obesity: Carrying extra weight, particularly around the abdomen, is a primary driver of insulin resistance.
- Physical Inactivity: Lack of regular exercise makes your muscles less sensitive to insulin, hindering glucose uptake.
- Family History: If a parent or sibling has Type 2 Diabetes, your risk increases considerably due to shared genetic factors.
- Age: The risk tends to increase as you get older, especially after age 45, though younger people are increasingly being diagnosed.
- Race and Ethnicity: Certain ethnic groups, including African Americans, Hispanic Americans, Native Americans, and Asian Americans, have higher rates of diagnosis.
Recognizing the Signs: Symptoms You Shouldn't Ignore
One tricky aspect of Type 2 Diabetes is that symptoms often develop slowly and can be subtle. Sometimes people live with high blood sugar for years without realizing it. However, if you notice several of the following changes, it's definitely time to schedule a check-up with your doctor.
Early detection is crucial because uncontrolled blood sugar can lead to serious long-term complications affecting the heart, eyes, kidneys, and nerves. Be mindful of these common indicators:
- Increased Thirst (Polydipsia) and Frequent Urination (Polyuria): As sugar builds up in your blood, your kidneys work overtime to filter and absorb the excess. When they can't keep up, the sugar is excreted into your urine, dragging fluids from your body, leading to dehydration and intense thirst.
- Unexplained Weight Loss: Despite eating normally or even more, your body may be unable to utilize glucose for energy, causing it to start breaking down muscle and fat for fuel instead.
- Extreme Fatigue: Since your cells aren't getting the glucose they need, you feel constantly tired and sluggish, even after resting.
- Blurred Vision: High blood sugar can pull fluid from the lenses of your eyes, affecting your ability to focus clearly.
- Slow-Healing Sores or Frequent Infections: High blood sugar impairs your immune system and affects blood flow, making minor cuts take longer to heal and increasing susceptibility to yeast or fungal infections.
Getting Diagnosed: The Simple Tests
Diagnosing Type 2 Diabetes is straightforward and requires simple blood tests. These tests measure the amount of glucose in your blood at different times or gauge your average blood sugar control over a few months.
The standard tools used by healthcare providers are reliable and minimally invasive. They help confirm the diagnosis and also determine the severity of the condition.
- A1C Test (Glycated Hemoglobin Test): This measures your average blood sugar level over the past two to three months. It's often used for screening and diagnosis and doesn't require fasting.
- Fasting Plasma Glucose (FPG) Test: This measures your blood sugar after you haven't eaten for at least eight hours (overnight fasting).
- Oral Glucose Tolerance Test (OGTT): This is a more involved test where your blood sugar is measured before and two hours after you drink a sugary liquid.
Taking Control: Managing Type 2 Diabetes Effectively
A diagnosis of Type 2 Diabetes doesn't mean your life has to stop. In fact, for many people, it becomes a catalyst for positive, sustainable lifestyle changes. Management is truly a partnership between you and your healthcare team.
The foundation of effective management rests on healthy habits, but sometimes medication is also necessary to reach target blood sugar levels. Keep in mind that consistency is key to long-term success.
Diet and Nutrition: Fueling Your Body Right
Nutrition is arguably the most powerful tool in managing Type 2 Diabetes. The goal isn't necessarily a restrictive diet, but rather a balanced approach that focuses on what and when you eat. Learning about carbohydrate counting and portion control can be life-changing.
Focus on whole, unprocessed foods that have a low glycemic index (GI). These foods cause a slower, steadier rise in blood sugar compared to highly refined items. Load up your plate with non-starchy vegetables, lean proteins, and healthy fats.
Limiting sugary drinks and excessive processed carbohydrates is essential. Furthermore, consult with a registered dietitian specializing in diabetes. They can create a personalized meal plan tailored to your lifestyle and specific medical needs.
The Power of Movement: Exercise Strategies
Physical activity is a powerful medicine for insulin resistance. When you exercise, your muscles use glucose for energy, even without much insulin. This dramatically lowers your blood sugar level almost immediately.
Aim for a combination of aerobic exercise (like brisk walking, swimming, or cycling) and resistance training (like lifting weights). Try to get at least 150 minutes of moderate-intensity activity per week. Even short, 10-minute bursts of movement throughout the day can make a difference.
Remember to always check your blood sugar before and after exercise, especially when starting a new routine, and keep a source of fast-acting carbohydrate nearby just in case.
Medication and Monitoring
For many individuals, lifestyle changes alone are not enough to maintain optimal blood sugar control. That's where medication comes in. The most common first-line medication is Metformin, which improves the body's sensitivity to insulin and reduces glucose production by the liver.
Your doctor may prescribe other oral medications or injectable medicines, including insulin, depending on how long you have had the disease and your specific medical profile. Regular self-monitoring of blood glucose (SMBG) is also a cornerstone of management.
Monitoring allows you to see how different foods, activities, and stress levels affect your blood sugar. Use this information, along with regular A1C checks, to adjust your management plan under the guidance of your care team. This constant feedback loop ensures you stay on track.
Managing Type 2 Diabetes is an ongoing process that requires commitment, but the benefits—increased energy, reduced risk of complications, and overall better health—are absolutely worth the effort.
Conclusion: Empowered Knowledge About Type 2 Diabetes
Navigating the world of Type 2 Diabetes might seem daunting initially, but remember that knowledge truly is power. We have covered the fundamental aspects: understanding insulin resistance, recognizing key symptoms, and embracing effective management strategies through diet, exercise, and medication.
The journey about Type 2 Diabetes is highly personal, but the principles remain the same: consistency, monitoring, and proactive collaboration with your healthcare providers. By making informed choices every day, you are actively working to control the condition rather than letting it control you. Take small steps today, and celebrate every victory on your path to better health.
Frequently Asked Questions (FAQ)
- What is the difference between Type 1 and Type 2 Diabetes?
- Type 1 Diabetes is an autoimmune condition where the body stops producing insulin completely, usually diagnosed in childhood or young adulthood. Type 2 Diabetes, which accounts for the vast majority of cases, is characterized by insulin resistance and usually develops over time due to lifestyle and genetic factors.
- Can Type 2 Diabetes be reversed?
- The term 'reversal' is sometimes used, but 'remission' is more accurate. Remission means achieving and maintaining normal blood sugar levels without medication. This is often possible, especially in early stages, through significant weight loss and major dietary changes. However, regular monitoring is always necessary, as the condition can return.
- How often should I monitor my blood sugar?
- Monitoring frequency varies based on your treatment plan. If you are on insulin or certain medications, you may need to check several times a day. If you manage the condition through diet and exercise alone, your doctor might recommend checking once a day or a few times a week, combined with routine A1C tests.
- What are the most serious long-term complications?
- Uncontrolled high blood sugar can damage blood vessels throughout the body, leading to serious complications such as heart disease (heart attacks and strokes), kidney failure, diabetic retinopathy (vision loss), and neuropathy (nerve damage, often in the feet).
About Type 2 Diabetes
About Type 2 Diabetes Wallpapers
Collection of about type 2 diabetes wallpapers for your desktop and mobile devices.
High-Quality About Type 2 Diabetes Photo Collection
Experience the crisp clarity of this stunning about type 2 diabetes image, available in high resolution for all your screens.

Breathtaking About Type 2 Diabetes View in 4K
Explore this high-quality about type 2 diabetes image, perfect for enhancing your desktop or mobile wallpaper.

Breathtaking About Type 2 Diabetes Landscape Photography
Transform your screen with this vivid about type 2 diabetes artwork, a true masterpiece of digital design.
Amazing About Type 2 Diabetes Landscape for Desktop
Explore this high-quality about type 2 diabetes image, perfect for enhancing your desktop or mobile wallpaper.

Breathtaking About Type 2 Diabetes Image Digital Art
Explore this high-quality about type 2 diabetes image, perfect for enhancing your desktop or mobile wallpaper.

Detailed About Type 2 Diabetes Landscape Photography
Experience the crisp clarity of this stunning about type 2 diabetes image, available in high resolution for all your screens.

Serene About Type 2 Diabetes Background in HD
Explore this high-quality about type 2 diabetes image, perfect for enhancing your desktop or mobile wallpaper.
High-Quality About Type 2 Diabetes Capture Art
Transform your screen with this vivid about type 2 diabetes artwork, a true masterpiece of digital design.
Amazing About Type 2 Diabetes Background for Mobile
Experience the crisp clarity of this stunning about type 2 diabetes image, available in high resolution for all your screens.

Mesmerizing About Type 2 Diabetes Image Illustration
Transform your screen with this vivid about type 2 diabetes artwork, a true masterpiece of digital design.

Gorgeous About Type 2 Diabetes Picture in 4K
Immerse yourself in the stunning details of this beautiful about type 2 diabetes wallpaper, designed for a captivating visual experience.

Spectacular About Type 2 Diabetes Photo for Mobile
A captivating about type 2 diabetes scene that brings tranquility and beauty to any device.

Gorgeous About Type 2 Diabetes Photo Illustration
This gorgeous about type 2 diabetes photo offers a breathtaking view, making it a perfect choice for your next wallpaper.

Dynamic About Type 2 Diabetes View in HD
Immerse yourself in the stunning details of this beautiful about type 2 diabetes wallpaper, designed for a captivating visual experience.
Mesmerizing About Type 2 Diabetes Picture for Desktop
Discover an amazing about type 2 diabetes background image, ideal for personalizing your devices with vibrant colors and intricate designs.

Mesmerizing About Type 2 Diabetes Background for Mobile
Explore this high-quality about type 2 diabetes image, perfect for enhancing your desktop or mobile wallpaper.
Stunning About Type 2 Diabetes Scene for Mobile
This gorgeous about type 2 diabetes photo offers a breathtaking view, making it a perfect choice for your next wallpaper.

Crisp About Type 2 Diabetes Landscape for Mobile
This gorgeous about type 2 diabetes photo offers a breathtaking view, making it a perfect choice for your next wallpaper.
Detailed About Type 2 Diabetes Moment Concept
Transform your screen with this vivid about type 2 diabetes artwork, a true masterpiece of digital design.

Mesmerizing About Type 2 Diabetes Picture Illustration
Experience the crisp clarity of this stunning about type 2 diabetes image, available in high resolution for all your screens.
Download these about type 2 diabetes wallpapers for free and use them on your desktop or mobile devices.